Introduction
We were delighted as our 12-year-old grandson ordered a Caesar salad when we were having dinner at a pizza place. Vegetables! However, the dinner was December 22, 2019, shortly after CDC and FDA issued yet another warning against eating romaine from Salinas, California. I asked the server where the romaine came from. He didn’t know but went in the back to inquire. He returned and said, “Salinas.”
Since 2017, seven outbreaks involving romaine lettuce have sickened hundreds and killed five. Those are the reported numbers. No one knows how many other people got sick. In six outbreaks the lettuce came from California’s Salinas Valley region; in the seventh from the Yuma, Arizona region, which includes California’s Imperial Valley. Repeated FDA and CDC warnings against eating romaine have left consumers adrift in a sea of confusing announcements, advisories, and recalls. Is romaine safe to eat?
Between November and March, almost all of the country’s romaine, iceberg, red leaf, green leaf, arugula, broccoli, and cauliflower (collectively known as leafy greens) comes from the Yuma region. During the rest of the year, leafy greens are grown in the Salinas region. The two states produce 98 percent of the country’s lettuce. Anyone who eats salad or likes lettuce on their Big Macs or tacos is personally impacted by how lettuce is grown and processed.
Most consumers will be surprised to learn what happens to their lettuce before they bring it home from the supermarket. Between lettuce farms and the ultimate consumer is a remarkable system of steps taken by farmers and processors to protect the safety of leafy greens. If an outbreak does occur, federal and state regulators employ an elaborate network of laboratories to identify the source of the contamination.
As a consequence, the chances of getting sick from eating leafy greens in America are minuscule. To put the risk in perspective, consider that California and Arizona farmers produce an estimated 130 million servings of leafy greens every day of the year.
Consumers should take comfort in knowing that farmers and processors, in response to the recent outbreaks, have implemented even more stringent standards. That said, there are inherent risks in eating raw food that is grown outdoors. The system is not and never will be perfect.
“I Wouldn’t Wish This on My Worst Enemy”
On March 20, 2018, Louise Fraser, a 66-year-old woman from Flemington, New Jersey, ate a Fuji Apple Chicken Salad at a Panera Restaurant in Raritan, New Jersey. Over the next few days, she experienced severe stomach cramps, nausea, vomiting, headache, and a fever. When her diarrhea turned bloody, she went to the emergency room at Hunterdon Medical Center. On March 25th, the medical team admitted her and began a battery of tests. Laboratory tests confirmed she was infected with E. coli O157:H7, which caused hemolytic uremic syndrome, a condition that can lead to kidney failure and death. It took 13 days of medical supervision and three blood transfusions to save her life. She calls the infection “the worst experience of my life. I wouldn’t wish this on my worst enemy.”
Louise became ill from an outbreak of E. coli O157:H7 traced to romaine grown in the Yuma region. The outbreak killed five people, hospitalized 96, and sickened 240 in 36 states, before ending in June 2018, making it the largest outbreak of this particularly nasty strain of E. coli since 2006.
Infectious Diseases and Food
Guide books warn travelers to third-world countries not to drink the water or eat raw vegetables for good reason. Due to the lack of adequate sanitation, the water is often contaminated with human or animal fecal matter, and farmers often use that water to grow vegetables.
Pathogens, including bacteria, fungi, and viruses, cause infectious diseases. E. coli O157:H7 most often occurs in the intestinal tracts of farmyard animals, especially cattle, sheep, pigs, and poultry. The animals suffer no symptoms, but they serve as carriers that shed bacteria in their feces, which can end up in the water supply. People can get sick from drinking contaminated water, but most E. coli infections come from eating food irrigated with the contaminated water.
Dozens of E. coli outbreaks associated with leafy greens have occurred since 1995. The worst one, in 2006, involved baby spinach that came from an organic farm in California’s Salinas Valley. That outbreak prompted the California and Arizona lettuce industries, in 2007, to enter Leafy Greens Marketing Agreements (LGMAs), which require members to comply with science-based guidelines for producing and harvesting leafy greens.
In 2011, Congress passed the Food Safety Modernization Act (FSMA), which adopted the best practices of the LGMAs. The Act strengthened the food safety system by broadening FDA’s authority and requiring FDA to promulgate science-based, minimum standards for the safe production and harvesting of fruits and vegetables.
Growing Lettuce: Food-Safety Challenges
Lettuce farmers face food-safety challenges greater than other food producers. Pasteurizing, irradiating or cooking kills pathogens in most foods. But there is no “kill step” for lettuce, which is grown outdoors, not in a controlled environment like a factory or a greenhouse, and eaten raw. Paul Brierley, head of the Yuma Center of Excellence for Desert Agriculture, describes farmers’ struggle against E. coli O157:H7 as “fighting an invisible, tasteless, odorless enemy.”
I first took students in my class, The Colorado River, on a field trip to Yuma in 2016. We met with a prominent farmer at his headquarters to learn about “food safety.” If a flock of geese fly over the farmer’s field, or a dog or deer wanders in, they may leave behind droppings with E.coli and other dangerous microbials. To monitor such intrusions, he keeps meticulous records of every occurrence and the response by date, time, and location. On his large conference room table, stacks of binders chronicled food safety steps from preparing the fields each season through planting and harvesting.
Food safety, whether in Salinas or Yuma, starts with a pre-harvest inspection of fields and fertilizers. As anyone with a backyard garden knows, manure helps things to grow. But it’s risky to use around vegetables. Before harvesting, food safety auditors (employed by shippers not growers) review a farmer’s policies and records, conduct a visual inspection of fields for signs of animal intrusion, and verify the practices are in place. The last step before harvesting involves taking samples from plants and sending them to a lab for testing. The usual practice is N60 or 60 samples in a five-acre plot.
Harvesting crews work for packing companies and follow elaborate food safety practices. Outside each porta-potty is hand sanitizer. Pickers wear gloves, masks and gowns, depending on whether lettuce is to be sold “naked” or processed. Workers cannot wear jewelry other than wedding bands or carry anything in their upper pockets. Every picker’s tools are numbered.
When crews harvest romaine for processing, they core and clean each head and place them bottom side up in boxes. They spray the boxes with water mixed with sodium hypochlorite and non-iodized salt to wash off latex, a naturally-occurring and harmless white-milky sap that oozes from the cuts. The spray helps to sanitize the cut surface, close the plants’ wounds, and prevent browning.

From Farm to Consumer
Harvested lettuce intended for processing is first sent to refrigerated warehouses, and vacuum cooled to 33-38 degrees F. At the processing plant, workers chop and shred the lettuce, which is sorted into different wash lines, for example, romaine in one and spinach in another. It’s usually triple-washed in flumes, each time with fresh water. Automated controllers inject sanitizer into the flumes for the first and second washes. The sanitizer prevents bacteria, such as E. coli O157:H7, that washes off a leaf from cross- contaminating other leaves during the washing cycle. The third wash involves a potable water rinse.
The washed lettuce is dried in large stainless-steel barrels using centrifugal force. Imagine a salad spinner that holds 300 pounds of lettuce. A machine then lifts the barrels and dumps the lettuce into a hopper, which feeds a conveyor belt to a scale, shaped like a cone with a bunch of buckets around it. A computer controls the buckets to measure the correct weight for each bag, depending on the customer’s needs.
Workers back-flush the bags with nitrogen to control the amount of oxygen in the bag. Processors use modified atmosphere packaging. I think of lettuce bags at my local Safeway as “plastic bags,” but processors regard them as oxygen transmission rate (OTR) film. One processor’s food safety director (who asked me not to use his name, so we’ll call him John Doe) explains that “the OTR film is specific for each type of lettuce and allows for an exchange of gases between the inside of the bag and the outside.” It allows just enough oxygen to induce the lettuce to go dormant. The lettuce remains in that state as it travels around the country until the bag is opened at a restaurant or a home.
Each bag is vacuum-sealed, run through a metal detector and hand-packed into boxes. At some processors, an inkjet printer stamps a label on every bag and box. Each label, explains Doe, “has a unique code with the production date, plant code, pack line production shift, the stock-keeping-unit (SKU) code, and a timestamp down to the second.” Workers place the boxes on pallets and load them onto refrigerated trucks.
Processors typically clean the entire plant every day. “Sanitation for us is the most important part of the day,” says Doe. “A crew of 20 cleans every belt, piece of cutting equipment, floors, drains, walls, everything. The process starts with a dry pick-up then a rinse, and the application of chlorinated alkaline soap. Workers foam and scrub the areas that need it, and finish up with a final sanitizer, either peracetic acid or quaternary ammonia. That’s done every night.” On weekends, he explains, they shut the plant down for “a deep clean period, from Sunday into Monday, when we do preventative maintenance that we can’t get done during the week.”
Shipper-processors sell to restaurant and grocery chains and foodservice companies, such as Sysco, which delivers to schools and hospitals. In a matter of hours or days, lettuce arrives at grocery stores around the country. Ironically, consumers may be the weakest link in the produce food safety system. What do you put on the seat in your grocery cart? Until recently, I put produce. Now I’m haunted by the image of the last customer’s dog, toddler, or purse. Once home, many consumers put lettuce into the sink or on a counter — two places loaded with bacteria.
A Mystery Fit for CSI
In early April 2018, the New Jersey health department contacted CDC about a cluster of E. coli O157: H7 infections. Many of the sick people had eaten salads at restaurants before becoming ill. In subsequent days, according to Dr. Laura Gieraltowski, an epidemiologist who heads CDC’s Foodborne Outbreak Response Team, “illnesses with the same DNA fingerprint were uploaded to CDC’s PulseNet database — indicating a potential multistate outbreak.”
PulseNet is a national network of 83 public health and food regulatory laboratories that submit samples of harmful bacteria from infected patients. FDA also employs another network, GenomeTrakr, which sequences the genomes of foodborne pathogens and uploads data to a publicly-accessible database. The two systems function symbiotically, one generating data about patients, the other about food.
Like a police detective looking at pins on a board in a murder investigation, Dr. Gieraltowski’s team looks for points of convergence from clusters of illness with a common point of exposure, such as a restaurant. FDA’s network of specialists tries to figure out the origin of the contaminated food. Their approach is to move backward from sick people through the food distribution system to the original supplier. This process, called a traceback, was exceedingly challenging in the April 2018 romaine outbreak.
Romaine is a perishable commodity with a short shelf life. By the time people get sick, physicians and clinics report their cases, laboratories test the specimens and fingerprint the pathogen, and health officials interview the sick people, the shelf life is over. Based on interviews with patients, clinical laboratory results, and DNA fingerprinting, FDA announced on April 13, 2018, that “the likely source” was farms in the Yuma growing region.
In June 2018, FDA investigators inspected farms, interviewed farmers and processors, and contacted cattle feeding operations and water districts. FDA teams were searching for the root cause of the outbreak. CDC’s National Antimicrobial Resistance Monitoring System (NARMS) laboratory used Whole Genome Sequencing (WGS) to determine that irrigation water from a Wellton-Mohawk Irrigation and Drainage District canal shared the same rare molecular fingerprint as the O157:H7 that infected the sick people. FDA found no other evidence of the presence of O157:H7.
To pinpoint precisely which farms and fields provided the romaine, investigators would need samples to test. However, by the time the FDA team arrived in Yuma, the romaine season had ended, the farm equipment cleaned and stored for the next season, and the processing plants closed down. There was no romaine to test. FDA did identify one farm that sent whole-head romaine to an Alaska prison where eight inmates got sick. In that case, the farm was the sole source supplier, but it did not cause the nationwide outbreak.
On November 1, 2018, FDA’s Environmental Assessment concluded the romaine came from the Yuma region. The traceback identified 36 fields on 23 farms that supplied romaine “that was potentially contaminated.” (Emphasis added). As seen on the Traceback Diagram (next page), multiple farms sent romaine to each processor, where the product became commingled as it was washed, dried, packed, and boxed. Distributors, in turn, received romaine from more than one processor. The commingling, FDA admitted, “made it impossible to definitively determine which farm or farms identified in the traceback supplied romaine lettuce contaminated with the E. coli O157:H7 outbreak strain.” That’s one reason why, on the Traceback Diagram, FDA redacted the names.
FDA’s assessment of the Yuma outbreak concluded that “the most likely way” romaine became contaminated was from the Wellton-Mohawk irrigation canal water because that’s the only place FDA found E. coli O157:H7. How did E. coli get into the water? FDA suspected the source was an adjacent Concentrated Animal Feeding Operation (CAFO). The Five Rivers Cattle, LLC feedyard in Wellton, Arizona, about 30 miles east of Yuma, can house more than 100,000 head of cattle at a time.
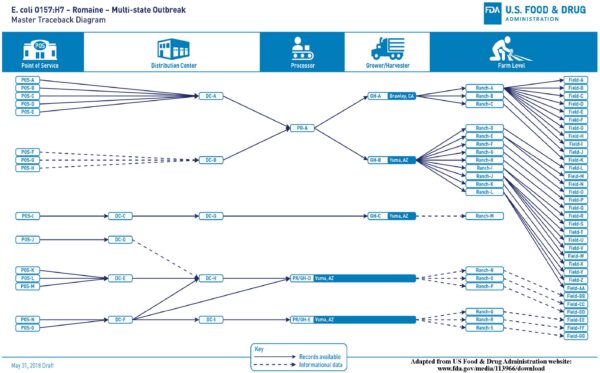
FDA Traceback Diagram

I asked Bill Marler, a leading food safety attorney, what he thinks caused the outbreak. Marler said the answer is obvious if you look at an aerial photo of the CAFO close to the canal. “It doesn’t take a rocket scientist to figure out the likely source of O157 in the Yuma valley. It’s cow shit.” He is hardly alone in reaching this conclusion, though several people expressed their views off-the-record. Manure is a vexing problem for feedlots: each steer can produce 65 pounds per day, most of which is water.
Nagging doubts remain. For example, if canal water contaminated romaine, why did it not also contaminate baby leaf, spinach or spring mix, which are irrigated with the same water. If canal water did not contaminate romaine leaves, is there another explanation? FDA ruled out wild animals because O157:H7 is an antibiotic-resistant strain, suggesting it came from the scat of domestic animals, who were inoculated or given feed with antibiotics in it.
FDA inspectors sampled soil, wild and domesticated animal scat, biological fertilizers, surface and subsurface water, irrigation water from the Colorado River, and sediment from irrigation canals. In the end, only three samples from the Wellton-Mohawk canal tested positive.
FDA also considered unusual weather patterns, including a hard freeze in February 2018 and strong winds in March 2018. The cold temperatures blistered romaine leaves, making the crop more susceptible to microbial contamination. High winds possibly carried contaminated soil particles and romaine — with creased, upturned leaves — may be more vulnerable to trapping airborne particles. Aerial applications of pesticides could have caused the problem if the water used to dilute the chemicals was contaminated. Perhaps a pesticide applicator drew water from the irrigation canal and then sprayed fields with contaminated water.
FDA acknowledged these other theories but found no evidence to support them. The bottom line is that Wellton-Mohawk canal water tested positive for E. coli O157:H7, which commonly occurs in cattle, and a giant feedlot was located next to that canal. The rest is inference.
Outbreaks in November and December 2019 caused by lettuce from Salinas spawned another plausible explanation for the root cause, which focuses on timing. Six of the seven outbreaks since 2017 occurred toward the end of the romaine season, whether in California or Arizona. When farmers rotate their crops, they often spread manure or composting materials in advance of planting — at a time when romaine is still in the ground in neighboring farms. Perhaps wind or water spread E. coli to the romaine fields.
A May 2020 FDA report on the November and December 2019 outbreaks concluded that “a potential contributing factor [was] the proximity of cattle to the produce fields.” The report was not referring to a massive CAFO but cattle grazing on public land on nearby hills — as far away as two miles from the romaine fields. This should send a shudder through ranchers and farmers across the West because the bucolic image of cattle grazing on a hillside is often visible from low-lying farms.
“We Don’t Know Exactly What to Fix.”
In April 2018, before FDA investigators arrived in Yuma, the leafy greens industry established task forces to examine current practices and propose reforms. For example, harvesters now clean and sanitize the equipment daily. Farmers and processors changed many practices, hoping that one or a combination would have an impact. “But we just don’t know,” explained John Doe, the food safety director. “And that’s the really frustrating thing for everybody. Our customers and really the entire U.S. public wants us to fix it, fix it, fix it. And we don’t know exactly what to fix.” Nonetheless, one processor decided to stop buying from farms within a mile of a CAFO. That processor also changed its pre-harvest sampling methodology from sampling five-acre plots to sampling every acre.
In 2019, the Leafy Greens Agreements began to require growers to treat all surface water used within 21 days of harvest. (Before that, sunlight exposes vegetables to enough UV radiation to kill almost all dangerous pathogens.) Dr. Jennifer McEntire, vice president of food safety for United Fresh Produce, a trade association, describes this change as “a fundamental shift” from testing water on an annual basis to “proactively treating water during the period closest to harvest.”
“Food Traceability @ the Speed of Thought”
On November 1, 2018, FDA then-Commissioner Scott Gottlieb called for the industry to standardize record-keeping and to use labels or other tools to improve traceability. Food safety records on many farms are hand-written notes. Some bags and boxes have labels that identify the variety, grower, field, and harvest date; others don’t. The lack of a uniform standard creates problems for fast traceback. United Fresh Produce’s Jennifer McEntire supports improved labels. “If we have true traceability, we could
pinpoint exactly what the problematic product was, who produced it, and when. We wouldn’t need a broad advisory.” Labels on romaine now include the growing region (Salinas or Yuma), which enabled FDA in November 2019 to limit its consumer warning to romaine from Salinas.
In December 2018, Frank Yiannas, a renowned food safety expert at Walmart, became FDA Deputy Commissioner for Food Policy and Response. At Walmart, Yiannas used blockchain, the best-known type of digital ledger technology, to track mangos from two farms in Mexico to two stores in the United States. In a pilot project, each participant in the supply chain put data on the blockchain, which linked the blocks of data and reduced traceback time to 2.2 seconds. Real-time traceability is the holy grail to Yiannas, who refers to it as “food traceability @ the speed of thought.”
In April 2019, Yiannas and FDA Acting Commissioner, Ned Sharpless, M.D., announced that FDA would enter a New Era of Smarter Food Safety, anchored by moving from largely paper-based data to a digital system, such as FedEx, Uber, and Amazon use to track the movement of trucks, ride sharing and delivery of packaged goods. The new era arrived in July 2020 with FDA’s Blueprint for Smarter Food Safety, which will encourage and incentivize the leafy greens industry to adopt tech-enabled traceability measures. The labels on bags and boxes of lettuce may soon have data stored on the cloud or blockchain.
But labels can improve traceability only if data gets saved. No matter how remarkable digital ledger technology is, it will promote traceability only if the shipping/receiving clerk at a restaurant or a supermarket scans the labels when the boxes arrive. Yuma farmer John Boelts notes that traceability breaks down in “the last mile to the consumer,” when supermarket workers or home cooks throw away the bags and boxes. At a public meeting on the New Era that FDA hosted in October 2019, Yiannas acknowledged this problem: “What matters most is what people do.” The behavior of everyone in the food industry, from farmers to servers, will ultimately determine the safety of our food.
In September 2020, FDA announced a proposed rule regulating recordkeeping that would require the leafy greens industry to keep records with Critical Tracking Events and Key Data Elements. Prompt traceability requires three conditions: uniform labels, interoperable data collection and storage, and unanimous participation by growers, processors, shippers, and buyers. Although this rule has many exemptions, it would go a long way toward creating those conditions.
Uniform labels and effective digital storage could dramatically reduce traceback times. Better data will not prevent the initial consumers of contaminated produce from becoming sick, but it could limit the scale of an outbreak by quickly determining the source of the contamination. Other current research is directed at prevention by achieving real-time detection of pathogens before the lettuce ever enters the food chain. Paul Brierley, head of the Yuma Center of Excellence for Desert Agriculture, has a research project involving biosensors, which would enable farmers to detect pathogens in water or in the processing plant. Brierley concedes: “We have a long way to go.”
In October and November 2020, FDA announced an investigation of three new outbreaks of E. coli O157:H7. Its traceback investigations were unable to determine a common source of the outbreaks.
What Should Consumers Do?
In the meantime, consumers face hard choices. They certainly should not stop eating romaine and other leafy greens. Nutritionists agree that we should eat more fruit and vegetables.
Consumers may choose to wash all lettuce, even the bagged and boxed mixes. Despite the elaborate precautions taken by processors, contaminated romaine made its way into the distribution system. In November 2018, FDA warned that washing “may reduce but will not eliminate [E. coli O157:H7] from romaine lettuce.” Despite this warning, I don’t plan to start washing lettuce that has already been triple washed.
Consumers have other choices, including buying organic produce. But it is worth remembering that the 2006 E. coli O157:H7 outbreak involved spinach from an organic farm. Other consumers may prefer to buy greenhouse-grown lettuce, which has not been implicated in recent outbreaks. But lettuce grown indoors is a niche market, not one capable of producing tens of millions of servings a day. Still others may want to buy from farmers markets. But it is unclear whether that lettuce is safer than processed lettuce from California or Arizona. Plus, few farmers markets are open from late fall through winter, which is the Yuma season. If you want lettuce during those five months, it’s going to come from Yuma.
When bad things happen, Americans expect that someone or something is to blame. We want everything to be perfect, whether it’s a medical procedure, a car repair, or the food we eat. However, no amount of testing and treating will completely eliminate the risk of getting sick from eating raw something that is grown outdoors.
